Metabolic syndrome and insulin resistance in the horse can be a real challenge for the horse owner and veterinarian to manage. It seems like there are several approaches offered online and from veterinarians, but often those therapies yield little for the horse in regards to clinical benefits. Most of these horses continue to suffer bouts of instability throughout the years, followed by periods of stability. Through a different approach, and seeing the problem for what it truly is, many of these horses can be helped on a whole new level. This approach is more of a lifestyle change than a true therapy, targeting cellular repair and rejuvenation to benefit the horse and return cellular function back to a baseline level.
Insulin resistance in the horse is ever-increasing with case loads rising each year. The problem is complex on a health level, but yet, not too difficult to understand. The key is to wrap your head around even a small facet of the problem, because then you have a better understanding of what you are doing and what your therapy goals are for your horse. As this begins to happen, then outcomes are much better in the short and long-term.
“Being ignorant of the causes leads to being more susceptible to the effects“
-Dr. P. Quimby
What is insulin resistance in the horse?

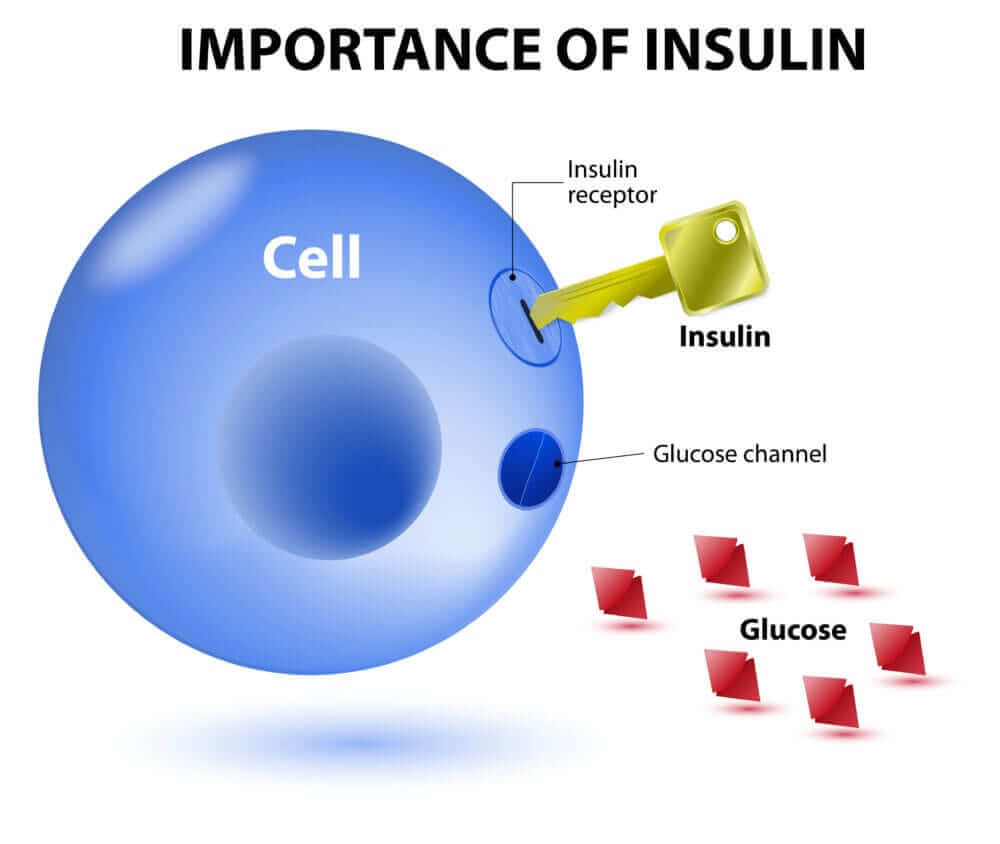
Insulin resistance is in simple terms, a state in which the insulin receptor on the surface of the cell is not working properly. As a result, not only can insulin not bind to this dysfunctional receptor, but it cannot therefore shuttle glucose or sugar into the cell for the purposes of energy generation. Insulin levels then begin to rise in the blood or serum and are detectable, due to not binding to the receptor properly. In most cases, based on human research which is applicable to equine health, the insulin receptor becomes dysfunctional or altered as a result of oxidative stress damage, which is really secondary to chronic inflammation in the horse.
What is the big deal and how does this impact your horse?
Insulin serves the main function of shuttling glucose or sugar into the cell for energy or ATP production. This energy is not just physical energy as in stamina, but is cellular energy needed for other biochemical pathways in the body including hormone production, digestive enzyme production, neurotransmitter function, organ function, circulation, overall tissue health, and endogenous (internal) antioxidant production. This is a pretty important concept to wrap your head around as a horse owner, mainly because this rise in insulin is NOT just a number on a laboratory form, but equates to an improperly functioning body and cellular structure.
The rise in insulin, due to inability to bind to the receptor in the horse, can create a multitude of issues, including:
- Impaired sugar/carbohydrate metabolism
- Impaired digestive health
- Impaired circulation
- Impaired tissue and joint health
- Impaired immune function
- Impaired performance and stamina
- Impaired cardiac and lung function (nitric oxide inhibition)
- Impaired antioxidant production in the body
As horse owners, and even veterinarians, we are all trained just to ‘see’ that insulin number, then assign a diagnosis of insulin resistance in the horse. In reality, we are missing the bigger picture and trying to make something really simple out of a very complex topic.
In order to truly see the problem of insulin resistance in the horse, you have to see the problem on a much bigger scale. Based on human research, which is applicable in the horse, insulin dysfunction is secondary to oxidative stress damage, which is involved with chronic inflammation. This chronic inflammation stems or originates from many locations, but one main area of focus is the digestive tract. The topic of digestive health and diet in the horse has been discussed in many other articles.
The reality is that oxidative stress damage is not just impacting the insulin receptor, but many other aspects of cellular health in the horse. This is evident in many insulin resistant horses as a high percentage also develop leptin resistance, which again is more oxidative stress damage to yet another receptor. This problem of oxidative stress damage goes much further, outside of these two hormones and includes generalized mitochondrial dysfunction, which means your horse’s cells in general are not working optimally. This then leads to the many issues mentioned above.
Just look at the average metabolic or insulin resistant horse. Connect the dots and see past just a number representing insulin on a piece of paper. Most of these horses are not just overweight, which is impaired metabolism, but many also have:
- Excess body weight
- Poor hoof condition
- Thrush/white line disease
- Tendon complaints
- Allergies
- Digestive upset
- Uveitis
- Non-healing wounds or injuries
- Heat intolerance
These are all linked in with altered cellular function, either impacting the immune response or tissue health by itself.
The bottom line….Your Horse is More Than Just an Insulin Reading or Number!
Insulin Resistance and Oxidative Stress in the Horse
Oxidative stress and damage from chronic inflammation is at the root of most problems in the average metabolic horse. This oxidative stress damage is ongoing in every horse, to various degrees, and impacts health and soundness. In many, the damage is reflected in normal cellular function, which includes insulin receptivity and glucose metabolism.
Oxidative stress damage occurs when there is an imbalance between free radicals and antioxidants. This can happen either in an excess or deficiency situation, which will be explained and presented in the next article. Free radicals are produced by your horse every time they take a breath, digest food, pump blood, or exercise. This is a natural part of their well-being and in reality, these free radicals produced naturally help to keep the body healthy, the immune response stimulated, and the horse’s body in balance.
Excess free radicals, in relation to antioxidant defenses, are the main problem. These excess free radicals can be secondary to excessive stress, exercise, improper diet, medications, unhealthy water sources, and even unhealthy forage or pasture. Pesticides, herbicides, pollutants, and even excess heavy metal levels in water and forage are key contributors. Medications also top the list, including vaccines, which are all considered xenobiotics and foreign to the body.
Pretty bad news, right? Well, there is always a light at the end of the tunnel. In this case, the good news is that the horse’s body, just like ours, naturally produces antioxidants internally to help buffer the ‘bad’ aspects of free radicals. The horse can produce vitamin C, glutathione (GSH), superoxide dismutase (SOD) and many other antioxidant-like chemicals internally, as long as nutrition and cellular health are optimal. In addition, many horse owners may supplement exogenous or external supplements with antioxidants which may range from vitamin C or E, to various herbs including Curcumin or others which tout antioxidant benefits. All good right?? Not really, unfortunately.
The average metabolic horse owner, and even the veterinarian, may recognize that inflammation and oxidative stress are at play in this condition, then feel that use of a plain antioxidant supplement or high doses of Vitamin E is sufficient. While this may be a good step in the right direction, it could actually turn around and be a bad thing. At the least, although it is a good effort, it likely is not sufficient to tackle the full problem. The concept of vitamin E usage was discussed in another article.
Oxidative Stress Damage, Insulin Resistance and Beyond in the Horse
When I evaluate a metabolic and insulin resistant horse, I dig much deeper and beyond just an insulin or even a leptin level reading. In my facility, which is available to any horse owner nationwide remotely, I perform fecal cultures to evaluate the health of the microbiome. I also evaluate their blood to determine free radical and antioxidant loads. What is seen now, in 2019, versus 8 years ago in our pilot research, is a little concerning.
In light of the above information, most of us would expect a horse with insulin resistance or metabolic syndrome to demonstrate high free radicals (d-ROM) and maybe normal or slightly low antioxidant levels (PAT). Seems logical, but for most, this is not the case. In fact, what we are seeing in our data is a below normal free radical (d-ROM) and also below normal antioxidant level (PAT), often very below normal levels. This situation, where both are low, is termed in the research community as “generalized cellular hyporeactivity“.
This situation is concerning, at least to me as a veterinarian and researcher, because it signifies significant cellular dysfunction. The cells in the body are not producing energy properly, not fueling pathways correctly, not producing natural free radicals that stimulate health, and are also not producing the natural antioxidants (GSH, SOD etc.) that help to protect the body. That then explains the other health ailments that many horses have, including immune compromise issues, tendon, joint and even hoof health problems. Cells are just not working properly and it leaves the horse’s body very vulnerable to many health and lameness problems.
So, there you have it. A major problem and this lack of properly functioning cells is due to chronic inflammatory damage inflicted over months and years of time. In order to restore health, this cellular function needs to be restored. This is what is behind the insulin resistance in the horse and takes it to a totally different degree and level.
Fixing the Cellular Problem in the Metabolic Horse
The instant fix that pops into most veterinarians and horse owners’ minds is that supplementation with antioxidants will remedy the problem. While this seems logical, it is not always the answer, at least in its simplest form. You have to remember two things here:
- The cells are damaged and not producing energy properly (ATP) and are not producing internal antioxidant defenses
- Most external sourced antioxidants (isolated form) require re-energizing by the body’s natural defenses to keep them from becoming free radicals.
This second point is very important and discussed in the Vitamin E article mentioned above. If you choose to give vitamin E or C or many other antioxidants to your horse, especially if in isolated form, your horse may benefit in the short term, but in the long-term there may do more harm. This is due to the fact that the horse may not be capable of recharging those antioxidants, which is done via internal defense mechanisms. If this does not take place, then those antioxidants you are giving to your horse may become free radicals, and contribute to more harm than good, creating further imbalance.
The solution or at least a better means of management is through the use of targeted antioxidants, specific chemicals really, which provide not just antioxidant support, but help to encourage cellular health and restoration. This is done through enhancing of mitochondrial function and health.
In addition, outside of the antioxidant situation, you have to keep in mind that the cells in the insulin resistant horse are not working properly, not generating energy, and just not functioning. Thus, it is crucial to restore energy pathways, and this can be accomplished by stimulating the horse’s body to use fats as an energy source. This pathway, although always present, is often put into a state of hibernation due to the constant intake of carbohydrates by the horse, much the same as in humans.
In order to better manage insulin resistance and metabolic syndrome in the horse, we have to take a higher approach, a cellular approach, which helps to tackle the root problems that are present. This, more often than not, leads to much better outcomes for the horse, in both the short and long-term.
These approaches and more details on insulin testing will be discussed in Part Two.
Author: Tom Schell, D.V.M., CVCH, CHN