Headshaking in the horse is a common problem and often affecting up to 30% of patients to variable levels, creating high frustration for the horse owner. The exact cause of this condition can be variable from patient to patient and thus treatment and results can be variable. Headshaking in the horse can vary in regards to presentation from simple flaring of the nostrils, flipping of the nose, rubbing the nose, snorting often, sneezing and even variable degrees of overt head shaking. Given the wide range of presentation, potential causes, lack of consistent treatment response and frustration factor for the horse owner, headshaking deserves some investigation for better management options. As is my character, let’s dig into what we know regarding headshaking and see if we can not only make sense of it, but also discover potentials for therapy.
If you have been around horses long enough, you have probably been witness to a horse that shakes his or her head. It could be while in the cross ties or just under saddle, or it may be while under stall confinement or even when turned out. Sometime it is response to another problem, such as pain, while in others it seems to be more attitude. The weird part to this condition is that it often takes a different variable to set one horse off over another. Some horses are worse during certain seasons and others may react to bright light. The question is why and what is causing the problem? Is it a behavioral issue or is there truly a pain response occurring, creating discomfort in some horses? As a veterinarian involved with equine rehabilitation, I have seen my fair share of these cases, all to different degrees with some being able to be eradicated, while others improved with management. They can be difficult and frustrating, but I believe that research and personal experience have much to lend in these situations, often producing better outcomes for management.
In many cases of headshaking, it does appear to be behavioral in origin in many of the horses that we have worked with. Often, in the patient’s history, there has been a prolonged period of stall confinement which increases stress to the patient and likewise vice development. This not only includes headshaking, but also weaving, cribbing and pawing. It is not uncommon to walk down the barn isle way on a race track or performance horse setting and see horses sticking the heads out of windows, weaving and headshaking. It is not the norm, by any stretch, but not an uncommon finding. These are developmental behavioral problems produced as a manifestation of their environment and stress, of which some patients are more sensitive than others. These patients tend to improve over time with change in their daily routine and also benefit from supplementation, which is discussed below, but again dependent on the individual patient and degree to which the condition has progressed over time.
In other cases, we do have direct problems with the patient, in which there is suspected nerve damage or increased nerve sensitivity, which can be related to allergies, trauma or even infections. Considering these causes, most horses with headshaking are thrown in to the category of ‘idiopathic headshaker’, which essentially means that we do not know the cause. This is what creates challenges in therapy in offering relief for patient and owner. If we knew the exact cause and could treat it properly, then our odds of providing relief are increased. This dilemma is encountered in many other conditions impacting health and despite not knowing the exact cause, if we look deeper into the pathophysiology behind the problem, there are options for better management.
Causes of Headshaking in the Horse
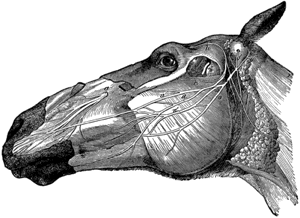
Headshaking is believed to be due to nerve irritation on a variable level, which can range from increased sensitivity to allergens to overt pain. The main nerve that is believed to be involved in the horse is the fifth cranial nerve called the Trigeminal nerve, which is involved with sensation and motor function of the face. In some equine studies, headshaking is more associated with specific branches of the Trigeminal nerve including the posterior ethmoidal nerve. Actually, the Trigeminal nerve has three main branches which are the opthalmic, maxillary and mandibular nerve. Headshaking in horses is believed to be closely related to Trigeminal neuralgia in humans, which demonstrates a range of problem from facial pain to migraine headaches.(1)
What is believed to be occurring is a hypersensitization of the Trigeminal nerve to stimuli, for various reasons. In cases of trauma, ear infections, guttural pouch infections or even cases of EPM, the cause of the potential nerve damage is obvious and with resolution of the primary problem, the headshaking often resolves or improves greatly. Given the close association of the Trigeminal nerve to the guttural pouch, ear and overall head, damage can occur easily and often secondarily to other problems. In some cases, the nerve sensitivity is associated with allergies such as allergic rhinitis, which may actually explain the seasonality of the condition. So, in those cases, we actually have two problems; an allergy and secondary nerve irritation.
The big issue outside of the known causes, is regarding what causes those ‘idiopathic cases’ in which no known cause can be found?

Anxiety and stress are in my opinion, one of the main contributors to idiopathic headshaking. Stress can be increased due to stall confinement, over training, poor diet influences and many other factors. Just like in the case of gastric ulcers, stress can be a major contributor to poor health on many levels. As stress increases, anxiety becomes a problem and often, just as in the case of humans or pets, an outlet for the pent up energy must be found. This is where often negative vices start and include headshaking, weaving, cribbing and pawing. In these patients, with routine diagnostics, no problem can be found and the behavior is variable from one instant to the next. We may have a horse that headshakes in the stall or cross ties, but when removed from that situation, the problem resolves. There may also be the patient that has been stall bound for several months with little to no turnout that develops the problems, but again resolves over time with increased turnout and socialization. The development of these negative vices as a result of stress in the horse is no different than finger nail biting, hair plucking, pacing or other OCD type of conditions in humans or even pets. It is a consequence of the environment and a result of anxiety.
So what about those cases that are not associated with anxiety, stress or have an underlying cause such as trauma or infection? The common denominator with the majority of headshakers appears to be involvement of the Trigeminal nerve and increased sensitivity to stimuli, but despite knowing this, the EXACT cause is yet to be determined and likely individual based.
In order to get to the ROOT of the problem, we have to understand what is occurring at a cellular level which may be triggering the increased sensitivity. The reality is that inflammation and even oxidative stress are found to be closely connected with headshaking, Trigeminal neuralgia and many other neuropathies in horses and humans. In many studies, it has been demonstrated that in cases of neuropathic pain and neuropathic dysfunction, even when caused by trauma or secondary to other health conditions such as diabetes, there is an increased level of pro-inflammatory cytokines including IL-1 beta, IL-6 and TNF-alpha. In one study, they not only demonstrated this fact, but also that the cytokines played a major role in the pathogenesis of nerve sensitivity.(2) In other studies, it has been demonstrated that patients with neuropathy have higher levels of free radicals and diminished levels of protective antioxidants. In fact, one study showed that neuralgia patients had lower levels of vitamin C, in which when supplemented, improved spontaneous pain response.(3)
So what is the big deal and what is the connection? Is the inflammation the primary problem or secondary? We don’t really know the answer to the second question, but when compared to normal, likely the level of inflammation and oxidative stress is reduced. What we do know is it is THIS inflammation and oxidative stress, whether if primary or secondary, that is creating nerve damage at a cellular level, leading to decreased normal function and possible increased sensitivity. What is the cause of the inflammation and oxidative stress? Many causes, ranging from impact of stress to infection to direct trauma. The question, when it comes to management, is “are we addressing these issues for maximal outcome?”
Management of Headshaking in the Horse
As is the case with many health conditions, we as patients, horse owners or pet owners seemed to fixated on the exact cause, looking for a precise diagnosis. In some cases, such as trauma or infection, the exact diagnosis is helpful as it can guide us with therapy. However, even with a case of headshaking secondary to EPM, we still have an underlying inflammatory, immune and oxidative stress component. If we do not address these, often the success rate with therapy is decreased and relapse rates can be higher.
Traditional therapies for headshaking mainly include the use of anti-histamines such as Cyproheptadine and in humans, they have used some anti-seizure medications and antidepressants, which have provided some relief but still are lacking in efficacy. In horses, Cyproheptadine has been noted to produce results in 70% of patients, but in my experience the results are much lower. The anti-histamines are believed to decrease nerve sensitivity to a degree and potentially modulate part of the immune response, but in most, they produce a level of drowsiness and even impact neurotransmitters, which may indeed actually be impacting anxiety and stress levels.
There are many types of antihistamines on the open market currently, and in truth, their level of effectiveness in the horse as a drug class are not very good. Thus, many use antihistamines to rule out allergies as a ’cause’ of headshaking and the results are poor, leading them to exclude allergies as a cause. This is not the case, because, as mentioned, antihistamines are not that effective overall in the horse and even if they were, they are not always effective against allergies or the allergic response, even in people. If they were, then we’d have a cure, right? But…we do not.
The question comes as to what happens in these patients if we attempt to modulate the stress levels, inflammation and oxidative stress?
In the study mentioned above, vitamin C supplementation in human patients was noted to decrease nerve pain response. The same has also been noted for use of the antioxidants Alpha Lipoic Acid and even Co-Enzyme Q10 in several studies. Curcumin has also been shown to provide anti-depressant, pain reducing and nerve protecting properties in many research trials. Considering that we have a strong inflammatory component, it begs the question as to what would happen if we controlled it better? In some studies, they have investigated the use of steroids and even NSAIDs with varying degrees of results in patients. It is true that these medication do impact inflammation, but only on a certain level and not as completely as we would desire. This is where Curcumin, Boswellia, Vitamin C, Vitamin E, CoQ10 and many others come into play as they impact the inflammatory pathway at a much higher level and reduce those damaging cytokines to a more normal level.
In one study, it was demonstrated that Curcumin changed the course of diabetic neuropathy, through mitigation of inflammation.(4) In another study, it was demonstrated that the concurrent use of vitamin C and vitamin E used together reduced neuropathic pain better than one by itself.(5) The increased results of using two antioxidant together to obtain better results is likely due to the fact that antioxidants themselves become free radicals in the process of neutralization. If we use several together, then they can actually recharge one another and minimize this effect. Even Spirulina blue green algae has been shown to have positive effects on reducing nerve sensitivity and being viewed as neuroprotective. (6)
Even when addressing strictly anxiety and stressed induced cases of headshaking, we can look to adaptogenic herbs such as Ashwagandha. Ashwagandha has been shown in several research trials to reduce clinical anxiety and impact of stress by reducing harmful cortisol levels. The other added benefit to Ashwagandha is that it has also demonstrated anti-inflammatory and antioxidant properties on the body, which may also account for some of the beneficial results.
A very popular formula for headshaking in the horse is the Cur-OST EQ Green, as this formula combines many of these nutrients and herbs, along with Curcumin, Boswellia, Spirulina blue green algae and Ashwagandha to detoxify and support nutrition in the horse’s body.
So, what’s the bottom line?
The reality is that headshaking in horses has many possible causes but actually one bottom line, which is inflammatory and oxidative stress damage that is occurring to the nerve cells, leading to increased sensitivity and reactivity. The precipitating factor can be trauma, infection, stress, allergies or many others but the bottom line problem is often the same. In reality, we have to ask if we can alleviate symptoms through use of targeted herbal and antioxidant therapy? The answer to this question is a simple “yes”, especially when we consider other invasive and potentially harmful options. It has been shown in many research trials and demonstrated in active practice.
In my years of clinical experience, we have alleviated about 85% of the symptoms in our patients. In many of those cases, we had underlying problems which were resolved, but in the majority, we had ‘idopathic headshakers’ that were often related to stress or other inflammatory problems present within the patient. We have managed them and improved them through the use of targeted herbal therapy and antioxidants, strictly. Several of those cases failed to respond to traditional modes of therapy, but benefited instead from our approach.
We do not rely on single herbs or antioxidants to impact headshaking, but instead use them together to increase the impact on the patient. The three main formulas that we have found success with include our Cur-OST EQ Green, EQ Total Support and addition of the EQ Adapt formula when needed, especially in cases of anxiety.
One last thing to note is a TCM or Traditional Chinese Medicine point of view on these conditions, from headshaking to allergies, which are often interconnected. They key here with many of theses cases is to note the time of occurrence during the year. In many, the conditions of allergies and headshaking worsen during the spring and summer. There are two factors here in the environment that are at play, being HEAT and HUMIDITY. This environmental heat will add to heat already present in the horse, which is heat itself and inflammation. When we add to it, we will bring it to the surface. Thus, many horses will exhibit clinical problems deriving from internal heat, which is worse during those times of the year. Then, we have the humidity factor, which adds to dampness present already inside of the horse, bringing it to the surface as clinical problems from laminitis to metabolic issues, allergies, headshaking, etc.
Given the above, from a TCM perspective, the solution through diet and herbs would be to ‘cool’ the body of the horse, or dry out the body of the horse, or both, depending on the situation. The Cur-OST EQ Green mentioned above does the first, cools the body and quenches the heat component. The Cur-OST EQ Total Support would do both, cool and dry out the body to a certain extent. Sometimes more cooling and drying is needed and we have to incorporate other herbal formulas like the Cur-OST EQ Tri-GUT or even the Cur-OST EQ IS formula.
One last note, the diet you are feeding your horse with headshaking is extremely important. Many diets with grains and synthetic based supplements such as vitamin-mineral blends, are actually harming the gut microbiome and creating more internal inflammation, heat, and dampness. ALL grains, no matter if you are feeding a commercial feed or something ‘clean’ like whole oats, ARE HEATING to the body of the horse. Thus, you will add more heat to the heat present. It is highly recommended to revamp the diet, remove the junk, no grains, and clean things up.
When we focus on health, often results begin to follow naturally as the body can function normally.
I hope this information helps! Feel free to let us know if you have questions as we are here to assist!
All my best,
Tom Schell, D.V.M.
Nouvelle Research, Inc.
www.nouvelleresearch.com
References:
Trigeminal Nerve Image in the Horse (Google Images)
1. Newton, SA et al. Headshaking in horses: possible aetopathogenesis suggested by the results of diagnostic tests and several regimens used in 20 cases. Equine vet journ. 2000. May 32(3)
2. Balkowlec-Isakra, E. Role of the immune system in inflammatory pain pathophysiology. Pol Merkur Lekarski, 2010, Dec 29(174)
3. Chen, JY et al. Vitamin C levels lower in neuralgia cases. Clin J Pain. 2009. Sept25 (7)
4. Li, Y et al. Curcumin attenuates diabetic neuropathy by downregulating TNF-alpha in a rat model. Int J Med Sci. 2013. 10(4)
5. Park, JM et al. Antiallodynic effects of vitamin C and E in chronic post ischemic pain rat model. Korean J Anes. 2013, Nov 65(5)
6. Patro, N et al. Indian J Exp Biol. 2011. Oct 49(10)


I am dealing with a head shaker and cannot figure if it’s coming from his neck. I’ve been down the road of CT scans, ruled out EPM. He always rubs his right nostril on his right knee, and yes, he’s had x-rays on his feet and legs and they are clean.Took my horse to Rood And riddle, they didn’t even come up with head shaker. I pretty much diagnose him myself through research. He is definitely worse in the spring and humidity. I am feeding him Tribute Essential k plus GC which is a ration balancer, I also give him 1 cup of alfalfa pellets, and he gets 1st cutting hay along with 2nd cutting with alfalfa and Orchard grass. What is the best kind of grain to feed him or ration balancer? I am afraid to totally take him off and only give him Hay, as he may not get all of his minerals and vitamins. He is a 5 year-old QH.
Hi Jacqueline, we offer plenty of information here to guide you with your horse from diet to supplements and gut health. Those are all playing a vital role in your horse. I would re-read this article and see if it can guide you further. If not, I am happy to look at your situation through a consultation and provide suggestions. The ‘key’ here is to realize that what you are doing currently, from diet to supplements, is not working. Then, you need to clean the slate and start over. https://secondvet.com/product/remote-equine-alternative-medicine-full-consultation/
Tom Schell, D.V.M.