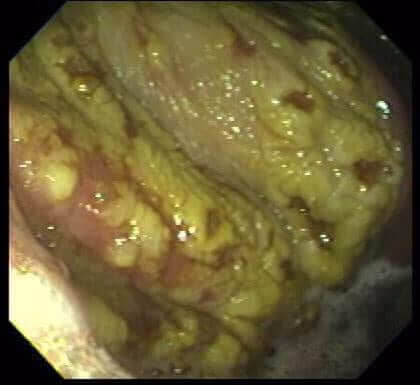
Stomach or gastric ulcers in horses are quite common, actually becoming more of a problem that in the past for our equine patients. It has been estimated that upwards of 80% of all horses, including sedentary and those in training, exhibit gastric ulcers but not all are clinically evident. In some studies, it has been demonstrated that just by moving a horse into a barn or training facility, the incidence of stomach ulcers increases beyond 80% and upwards to almost 100%. Some cases of ulcers are obvious with typical clinical signs, while others are more ‘quiet’ in nature and often only diagnosed incidentally. The sad part is that for many of these horses, they live a life on constant ulcer medications to control the clinical symptoms, which is not solving the problem but also costing the owner money and even, based on some studies, potentially inflicting harm. We need to dig deeper to find better ways of managing this problem in the equine industry.

For several years now, I have discussed the connection between stress and gastric ulcers, not only in horses but in humans. The connection is obvious and well known in human literature, but for some reason, we fail to make the connection with horses or maybe we just disregard it. One of the most common reasons for veterinary consultations, at least on my end, are gastric ulcers and how to best manage them in the horse. In many of these consults, the horses have been on multiple courses of medications, which include antacids, H2 blockers, and proton-pump inhibitors (PPI’s), which usually have improved the situation, but the horses need to remain on low doses or frequent high dose usage. This is a costly approach and again, potentially harmful, as we really do not know the long term consequences of these medications and on the human side, the long term effects are just now starting to become evident. I often discuss the impact of stress with the horse owners and try to put into motion regimens to curtail the effects, including; dietary modifications, herbal supplementation, and lifestyle changes. Many horses respond to these regimens, but in others the full changes cannot be implemented for various reasons and problems recurr.
In my years of study and equine research, I have communicated with many horse owners about the overall importance of GI health and how this plays into various problems in the horse. We have discussed hindgut health, hindgut ulcers, leaky gut syndrome and even bacterial imbalances, all of which contribute on some level to the issues facing our horses today. These are all pieces of the huge puzzle that we are trying to put together, to ultimately benefit the horse, but it is a slow process which many are not willing to undertake. Domestication of the horse and the huge demands we place on them are all major players in the game of ulcers, each contributing on some level. As long as these demands and human interventions in regards to lifestyle continue, no matter what we do, ulcers and health issues will remain, as this is something we have created.
The reality is that many of the medications on the market today do provide ‘relief’ for the patients, but in essence, through the use of these medications we are believing that the problem lies in gastric hyperacidity or over production of gastric acid, which then leads to the ulcer development. That is what these medications are treating, hyperacidity. Actually, over production of acid is uncommon and more relative to stress or other triggers, meaning that in most cases of ulcers, excess acid production within the stomach is NOT the problem. The acid is an irritant to the ulcer, but more often is not the actual cause. Stomach acid is vital to digestion and even protection against bacterial infections. By taking this viewpoint, through the use of these medications, we are not only NOT addressing the problem, but may actually be creating more harm by reducing a normal function of the body.
As I sat at my desk today, going through a stack of veterinary journals that tend to accumulate, I was pleasantly surprised to read an editorial article in the December 2015 issue of Equine Veterinary Education. The article was by Dr. Derek Knottenbelt of the University of Liverpool, UK. The title of the editorial was “Does significant gastrointestinal disease begin at the cardia and end at the pylorus?”. Essentially, the cardia is the first section of stomach, where the esophagus and stomach meet, while the pylorus is the end section of the stomach where the stomach and duodenum join. So, in reality, he is asking if significant GI disease is just localized to the stomach region? The editorial discusses, from Dr. Knottenbelt’s point of view, how the prevalence of gastric ulcers is on the rise and incidentally the risk is higher with more demands placed on the horse. Despite the heavy use of pharmaceutical medications, the ulcer problems in most horses continue, requiring daily dosing, which is really an ethical dilemma for us as veterinarians. As veterinarians, we took an oath to prevent animal suffering and cure disease, but in the case of gastric ulcers, we are more or less treating clinical signs and more so avoiding or not addressing the problem at hand. Dr. Knottenbelt is really asking if this is the best methodology for solving this problem or more so if due to heavy marketing and drug overuse, there is no initiative or drive to seek the true cause of the disease.
I quote Dr. Knottenbelt in his saying “We need to address the causes of disease and reduce our emphasis on developing more and more sophisticated, expensive and often performance limiting medications and procedures required to maintain high end performance.” I applaud Dr. Knottenbelt for saying this and wish all to often that others would feel the same and actually express it to one another. We seem to be caught up in this vicious circle of disease and pharmaceutical intervention, wherein the problem is rarely corrected.
The point to the article or editorial was that Dr. Knottenbelt is commenting on how the GI tract as a whole is an important component to equine health, potentially contributing to the ulcers we may see in the stomach, but also to other health issues. He comments about equine idiopathic bowel disease as being a problem based on rectal biopsies, as well as possible hindgut ulcers, acidosis and even colics as indicators that there is a problem there, but needs to be found. Dr. Knottenbelt further comments that maybe those horses that we actually diagnose with large bowel disease are only the tip of the iceberg, as it is possible that the higher percentage of horses have the problems but yet either go undiagnosed or are not clinical with evident disease. In fact, a large percentage of clinically normal horses have been shown to have subclinical large bowel disease. This is something that we have investigated in our fecal research studies at Nouvelle Research, Inc., noting that many horses which have no clinical problems demonstrate potentially harmful bacteria shifts within the feces which may open the door for problems. We note this to be obvious in those horses with clinical problems such as ulcers or laminitis, but quickly forget that many clinically normal horses also have the problem, but for some reason, it has not been triggered or activated. This helps to explain why some horses are more prone to laminitis during spring or summer, but in the ‘off season’, they become almost clinically normal. The problem is still there, just not activated likely by the high carbohydrate intake with the lush pastures.
In his final comments, Dr. Knottenbelt notes “simply because we have an endoscope and a drug that possibly helps to relieve the clinical signs of gastric ulceration, it surely does not mean that we can forget the causation and the need to address it. We should be focusing attention away from the treatment of gastric ulceration to it’s prevention so that drugs are not required to keep horses ‘healthy’, as by definition, a patient receiving drugs for a pathological disease cannot be considered healthy, even if the drug is effective.”
Again, I applaude Dr. Knottenbelt for his comments and could not agree more. I have always stated that “health is the abscence of disease and therefore, disease is the abscence of health“. This is true for many if not all medical conditions impacting animals or humans. Thus, the goal is to restore health, ideally in a drug free manner. It is rare to have a disease that is caused by a deficiency of any one medication, but more so the disease is often due to lack of proper diet and environmental factors, which need to be corrected in order to regain normal homeostasis.
In the end, gastric ulcers in any equine discipline are a difficult condition to manage with some being more receptive to therapy than others. We need to look beyond the medications and seek true answers. The connection with the GI tract and specifically the hindgut in the horse is an important one and an issue that we have discussed in prior articles.
https://nouvelleresearch.com/index.php/articles/385-leaky-gut-syndrome-health-soundness
https://nouvelleresearch.com/index.php/articles/341-managing-gastric-ulcers
This connection is not unique to the horse but also present in humans, however, it is complex and often multifactorial in nature. We continue to explore many options in our research, including the impact of bacterial shifts or dysbiosis in the horse. Many things to yet discover, but with time, hopefully we will have more answers.
In the meantime, in all of my equine patients with gastric ulcers, with or without clinical signs, I heavily rely on two herbal formulas in our approaches, which have proven to benefit over 90% of patients in less than one week, without medications such as omeprazole. My approach consists of addressing stomach and digestive health, while also modifying the internal stress response:
- Cur-OST EQ Adapt & Calm
- Cur-OST EQ Adapt & Recover
- Cur-OST EQ Stomach
Author: Tom Schell, D.V.M., CVCH, CHN