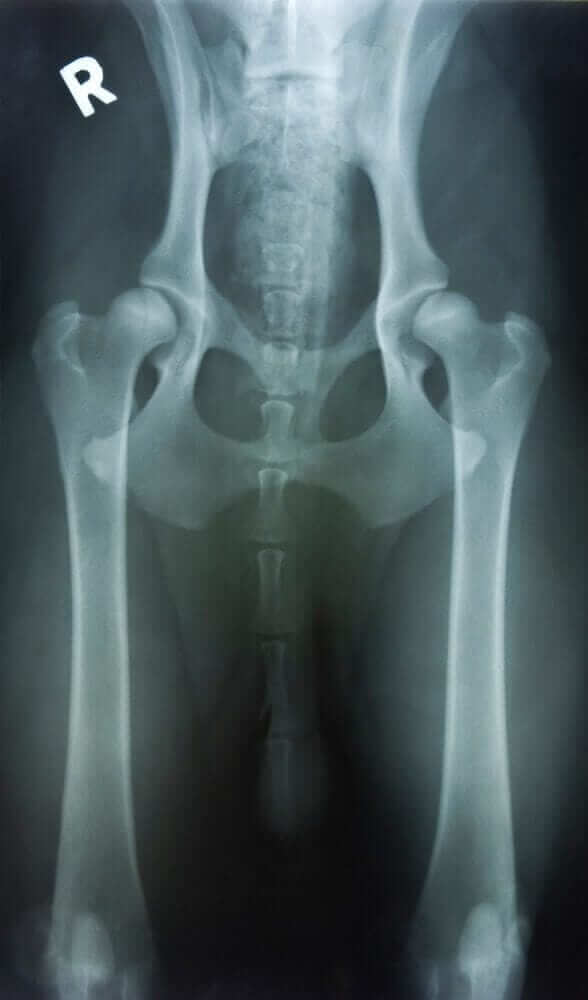
Our canine companions are not immune to joint concerns, but like us, they often live with day to day discomfort and pain. A dog wants to go, jump and play, but are limited in what they can do. The hips and back are main sources of problems in the dog, creating moderate pain, limited range of motion and a modest dependence on pharmaceutical medications just to keep them moving. Their problems are very similar to ours, as humans. We have choices when it comes to health care for our pets and options which may provide a higher level of quality of life. All we have to do is understand the process and see the possibilities.
A dog and a human are actually more similar than we are dissimilar. We have almost the identical body, just oriented differently, from bones to major organs, with slight variations. Like us, dogs are prone to joint disease with the major areas being affected including the lower back, knees and hips. Quite similar to us, as humans, actually. Joints are joints, no matter what species we are talking about. Over time, with increased stress, wear and tear, those joints are susceptible to break down and arthritis development. As the condition progresses, pain becomes a tremendous factor, impacting quality of life and creating a dependency on medications.
Just like in humans, certain factors contribute to joint problems in a dog, making them more likely to occur over time. These factors include:
- Genetics (breed)
- Conformational flaws
- Diet
- Body Condition
- Lifestyle factors
Almost any joint can be impacted by arthritis and degeneration in the dog, but the most common complaints usually stem from the hips, knees and lower back. In a prior article, we discussed the knee or stifle, with the most common condition occuring there being cruciate ligament disease.
The Hips and Pain in Dogs

The hips in the dog are very similar to our own, just oriented in a different plane, really as if we were down on all 4 limbs, walking around, instead of being upright. The hip joint is really where the ball or head of the femur, interacts with the acetabulum or cup of the pelvis. It is really like a ball sitting and rotating, perfectly fitting inside of a cup. This cup and ball junction forms the hip joint and the ball of the femur is held in place by a centrally located ligament, called the ligament of the head of the femur. This keeps things in place, preventing the ball from jumping out of its socket. Being a joint, this entire unit is then encapsulated by a joint capsule, containing joint fluid inside to improve lubrication and reduce friction. The ball and socket are both covered with cartilage, which protects the bone underneath and helps to absorb forces, not to mention glide smoothly. Friction is the enemy of joints. With more use and stress to a joint, inflammation increases. As the inflammation rises, the joint actually begins to produce less joint fluid in the long term and with this comes more friction and heat. Over time, that level of inflammation rises further and soon, cartilage degenerates and bone is impacted, leading to the development of arthritis.
When we are talking about the hip and arthritis, there is really two forms; general arthritis and hip dysplasia. It is important to discriminate between the two. Hip Dysplasia is a hereditary condition, genetic. It is more evident in larger breed dogs, including the Labrador, Golden Retriever, German Shepherd and a few other breeds. Hip dysplasia is a genetic condition where the ball of the femur and/or the acetabulum (cup) of the pelvis are not formed properly. Often times the ball is not as round as it should, being more oblong in shape. In other cases, the acetabulum or cup is rather shallow, not being able to contain the head of the femur very well. Hip dysplasia is diagnosed when the dogs are young, often with the initial clinical problems being evident before the dogs are 6 months old. Essentially, it is a young dog condition.
On the converse side, we have generalized hip osteoarthritis, which is typical arthritis impacting the hip as the dog ages. Really no different than in humans. In most cases of generalized hip arthritis, the initial diagnosis may be in the age range of 4-5 years of age in the larger breed dogs. It is important to distinguish between the two, as often we have a diagnosis of ‘hip dysplasia’ but our pet is actually aged out and is more in the group of generalized arthritis.
When it comes to actual, true hip dysplasia, we are often limited in options dependent on how bad the hips are deformed. In many of these cases, we can assist these patients over many months or even years, but all too often, the only true solution is a hip replacement. However, with generalized arthritis, our options of therapy to assist in managment for that patient, are greater, especially if we intervene at an early stage.
Lower Back Conditions in Canine Companions
The lower back in dogs is just a prone to problems as it is in humans. In this region, the most common complaints are discospondylitis and spondylosis.
The vertebrae in our backs are numerous and separated from each other by discs, which really are like fluid filled donuts, taking concussion forces and allowing the vertebrae to flex and move. In certain situations, those discs can rupture or herniate, in which case the fluid outpouching can then put pressure on nerves or even the spinal cord. Certain breeds that have longer backs, such as Beagles, Dachsunds and Basset Hounds are more susceptible to this condition. Any breed is really susceptible, especially with age related degeneration to the discs themselves. Clinical signs don’t always include back pain, but more so the pain is involving a leg due to sciatic nerve impingement or even more notably, the pets often drag a rear foot or a whole leg, or usually both legs. In many of these cases, especially if advanced, surgery is the only viable option in order to attempt decompression.
Spondylosis is really a form of arthritis of the lumbar vertebrae. What happens here is actually similar to any other joint. The cartilage surface begins to breakdown due to wear, tear and inflammation. As this condition progresses, bone spurs begin to form and can actually bridge the gap between vertebrae, connecting to the next one down the line. This bridging then leads to limited range of motion and contributes to significant back pain in some cases. If the condition gets severe enough, nerves can be compromised and with this function is impaired.
Therapy Considerations for Dogs with Back and Hip Pain
In many cases of both hip and back problems, many of these pets are on pharmaceutical medications each day to control clinical signs. The most common type of medication utilized as a first option are NSAIDs or non-steroidal anti-inflammatory medications. This group of medications can prove helpful in managing discomfort and pain, improving quality of life, especially in the early stages, but they are limited in their function and can have significant side effects, along with requiring frequent bloodwork monitoring. As the conditions progress, we start to utilize medications such as steroids or even narcotic medications. As a veterinarian, I would often prescribe the NSAID medications, but rarely had a need to employ the steroids or narcotics, unless it was a really advanced case.
More so, I opted to incorporate ‘alternative’ options, not just including herbs but also the diet and recommending exercise for the patient. Many of these pets are sedentary in their lifestyle, which encourages weight gain and overall stiffness of the joints. If we could alter the diet, make it more clean, less processed, higher nutritive value, then the patient would actually lose weight, which would take stress off of those joints and improve quality of life.
I feel herbs are very beneficial in these cases, not only for nutritive capabilities but more so their medicinal effects. Inflammation is the main factor we are attempting to balance, as in these patients it is at a higher level, which is contributing not only to their pain but joint degeneration as well. The medications mentioned above target pain, really, impacting the actual inflammatory process on a restricted level. They also have moderate side effects ranging from upset stomach to organ failure, not too mention their high cost.
Many herbs can assist us in better management in these cases, reducing or even eliminating the need for those medications. In reality, through the use of herbs we accomplish several things. First, we help to balance the inflammatory process and reduce discomfort. Second, we impact cellular health, which may aid in healing, strength and even metabolism, which then impacts energy and even weight. More often than not, with the proper use of herbs, the patients feel better overall, their discomfort is more managed, less pain and more energy overall.
When it comes to herbs, obvious ones such as Curcumin or Boswellia can help us to balance that inflammatory response and improve comfort, however, we cannot forget about the many others. Herbs such as alfalfa, spirulina and various medicinal mushrooms also have anti-inflammatory benefits, but also provide beneficial nutrients for cellular health and even aid in moisturizing the body to an exent, which is a problem as we age.
In our patients, the most common formula that I would use is our Cur-OST SA, which incorporates several herbs not just to address inflammation but support overall health. We would use this formula in almost any case of joint conditions and experienced good results in a high majority. In those patients that are larger, heavier body weights such as the large breed pets, the Cur-OST SA Pure is a another option as it allows for a lower dose, but does not provide the overall health balance as seen in the Cur-OST SA. In those pets that also have allergies, we would utilize our Cur-OST SA Total Support, to aid in balancing the inflammation response, but also address underlying gastrointestinal issues which may be contributing to both the allergies and joint concerns.
In all of these cases, a cure is not the goal, and rarely achieved even with surgical intervention. What we are trying to do is improve quality of life and reduce or better manage discomfort, as well as some of the cellular processes which may contribute to the condition. I do believe, that with proper management utilizing diet, exercise and herbal therapy, many of these patients can do extremely well.
Thank you.
Tom Schell, D.V.M.
Nouvelle Research, Inc.
www.nouvelleresearch.com