Itching, scratching, coughing, red eyes, hair loss and oozing skin bumps….all related to allergic conditions in horses and a common occurrence. Current approaches to therapy in allergies are often complex and unrewarding, leading to the condition becoming worse with every passing year, fluctuating from season to season. All of these clinical signs are evidence of a deeper seated problem in the horse, and through a better understanding you can take a different approach which often yields better management. As with most issues though, in regards to chronic disease in the horse, you have to see the root, the cause, and not so much focus on the clinical signs that are present.
Equine allergies are becoming more prevalent in today’s society, seeming to increase exponentially with every year in the average equine veterinary practice. Why? This is a question we must ask ourselves. It is not just in the horse, but in companion pets, and us. The rate of occurrence is increasing, which is evident by the high rate of usage of over the counter antihistamines. Again, we must ask why? The solutions being provided are not yielding answers, but simply covering up clinical signs or more so, really just improving them for most. Are allergies a sign of something deeper? Are they a sign of something more serious to come? Potentially.
What is an allergy?
An allergy is an inappropriate and damaging immune response to an allergen, which is something that is otherwise not considered harmful to the body. In most cases, the allergen can be a food protein, pollen, dust, dander and even some medications. Usually, these allergens are not deemed to be harmful, but for some reason, the horse’s body is mounting an immune response as if there were a formal invasion. Through this response, the process of inflammation is triggered to various degrees, impacting and altering cell function in the horse. Through this, we have clinical signs such as redness, itching, hives, mucous production and coughing. These are all inflammatory responses, in an attempt for the body to protect itself and get rid of the ‘invader’. Many times, we will have secondary problems such as infections which will develop due to host response being damaged. This is evident as skin infections, eyes infections and even lung (pulmonary) infections, all secondary to the primary problem, being the allergy.
Allergies are a broad topic, encompassing many possibilities. However, there are many common clinical situations in which they present in the horse, including:
- Superficial dermatitis (hair loss, pustules, bumps, redness, itching)
- Contact dermatitis (same as above, but related to a contact allergy with insects, plants or even topical sprays)
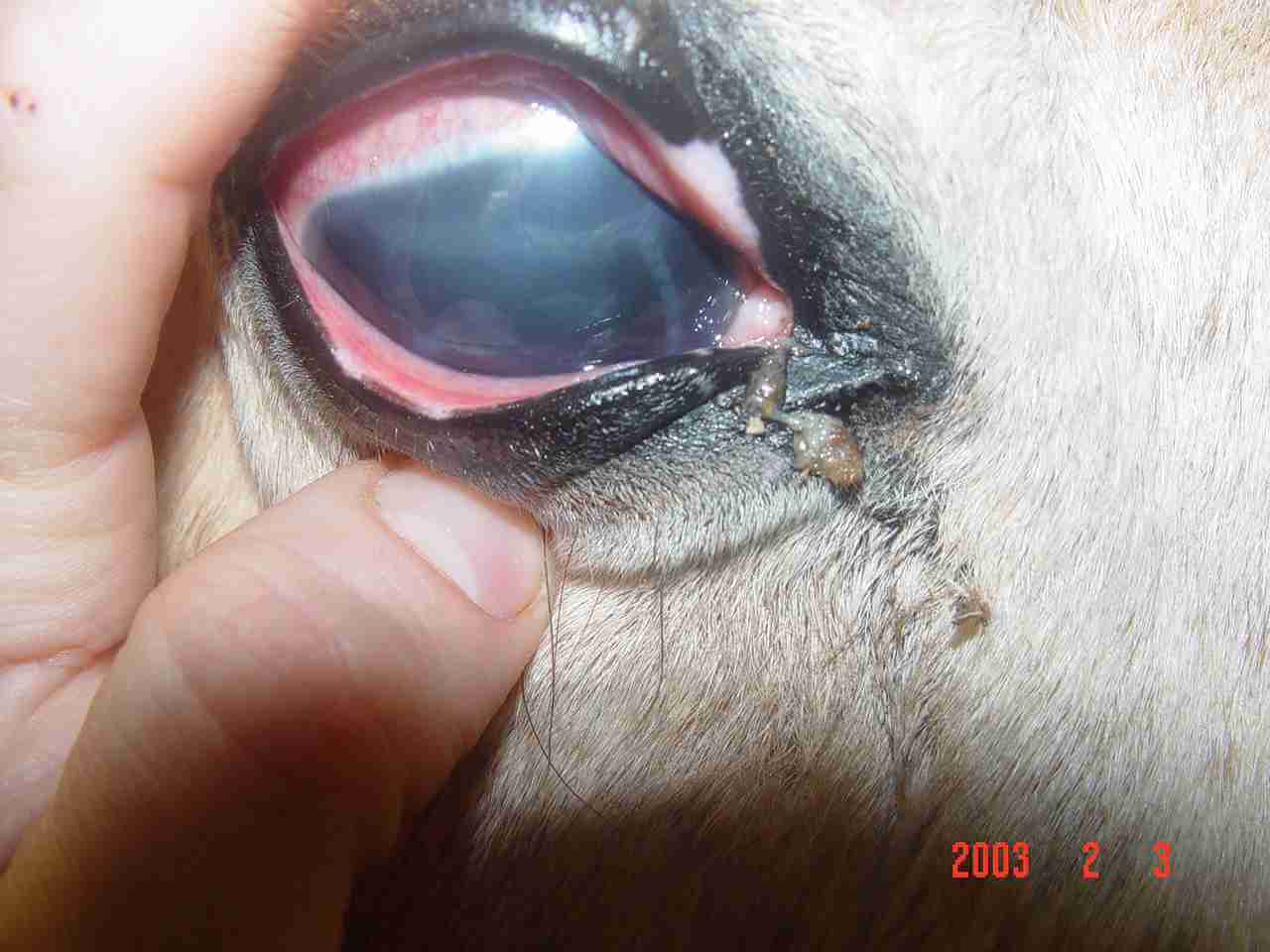
- Conjunctivitiis/keratitis (eye allergy with redness, discharge, squinting and tearing)
- Inflammatory airway disease
- Chronic obstructive pulmonary disease
- Vaccine and drug reactions
Underlying Connections & Causes of Allergies in the Horse:
Allergies are complex and some horses are more predisposed to them than others. Some go through life being miserable, dependent on the season, while others never seem to have a problem. This can be true for horses on the same exact regimen, dietary and training. There are many variables that play a role and include genetics, body condition, temperament, diet and the influence of inflammation and immune function. These factors can vary from one horse to the next and interestingly enough, each factor can and does then influence others.
In horses, much the same as in people and pets, we have different body types. Some are lean and some are overweight. Some are hard keepers with high metabolic rates, while others are deemed easy keepers, with a likewise slower metabolic rate. Both types can be impacted by allergies, but more commonly, what we see is that a high percentage of allergy patients are easy keeper horses. Not always true, but they represent a high percentage of the population.
Human research has shed light on many possible connections and causes to allergies. On a basic level, what we have to understand is that the presence of an allergy signifies two things: dysfunctional immune response and inflammation. One can cause the other and it is hard to say exactly which came first. Regardless, both are present and at a heightened level in those patients. What we have to do is look at potential connections, creators of the cascade of events.
The immune response is easily influenced by inflammation and the home base for the immune response is the gastrointestinal tract. What happens, in regard to health in the GI tract, is often then reflected throughout the body impacting the immune response. This is true in all animal species, including humans. However, we can have a primary problem there, such as underlying gastrointestinal dysfunction, or a secondary influence, such as inflammation. Again, one can influence and impact the other.
In almost all cases of allergies in the horse, in my experience, we have a problem in the GI tract, question is to what degree.
A leaner horse often has stress induced dysfunction of the GI tract, which then can contribute to inflammation, immune problems and allergies. The easier keeper type tends to have more primary underlying GI dysfunction, such as acidosis, irritable bowel conditions, poor digestion and even leaky gut syndrome, which then all contribute to inflammation and immune concerns. The bottom line is that in most, we have a breakdown on the gut level, problems in that area that are strongly contributing to the allergic response.
It is not just the gas, bloating, ulcers or even loose stools that are the concern, as these are all clinical signs. More so, we have variable changes on a cellular level, in response to inflammation, which can result in alterations or shifts to bacterial populations, impaired digestion/nutrient absorption and breakdown of normal barriers. One example would be ‘leaky gut syndrome‘ in which case the normal mucosal lining of the GI tract becomes damaged, more leaky or permeable due to tight cell junctions being compromised. This barrier is designed to protect, keep out unwanted material from having access to the rest of the body. As the barrier breaks down, certain food proteins, chemicals in foods (dyes/preservatives) and even bacteria can then access the blood stream. When this happens, the body can mount a tremendous immune and likewise inflammatory response, which over time can put the immune response on alert, contributing to the over-reactivity that is present in allergies.
There are many factors that contribute to this GI dysfunction, which include:
- Genetics (easy keepers)
- Stress (mental and physical)
- Diet and Nutrition
- Medications
- Personality
All of these factors interplay and one or many are present in each and every allergy patient.
Current Approaches to Allergies and Why They Fail in the Horse
Our current approaches to allergies in the horse are at best covering up or managing symptoms. We live in a world defined by medications, looking for the next pill or injection that will ‘cure’ what ails us or our animals. Simply put, these medications are doing little to relieve suffering and resolve the increasing prevalence of allergic conditions in the horse.
In most cases, an allergic condition is not hard to diagnose or even suspect. They are obvious in the case of acute development of hives, as seen with a bee sting or even topical application of a reactive fly spray, but not so obvious when it comes to chronic hair loss or even a cough. This is where diagnostics come into play, but even they can be misleading. In all cases, I do believe that routine bloodwork is necessary to assess a full clinical picture of the patient. In most, these values are normal, unless we have a more severe secondary infection or other health problem. One common practice that is being done more and more, to document allergies, is allergy testing which can be done with blood or via allergen injections. Even here, results can be misleading.
Allergy testing is done either via blood evaluation or by individual allergen injection. What is being determined is the response by the immune system in that patient, when faced with various allergens. An inappropriate immune response to an allergen results in a positive test or a hive development of a specific size after allergen injections. As a result of this allergy testing, we then try to eliminate positive allergens from the environment or create hypersensitivity injections, acting as vaccines to hopefully quiet the immune response down. We hope that then through this elimination, the allergy will be resolved. Improper thinking.
Why is allergy testing misleading? Personally, I have done very little allergy testing in equine patients for the sole reason that it is costly and provides me with very little information that will benefit that patient. Most times, an allergic situation is highly suspected, and testing is not needed to verify that fact. Due to cost of testing, I am more focused on using funds in the most efficient way, and in most it does not include allergy testing.
What I find misleading is that in most cases, we will see that the equine patient is allergic to allergens that are a part of their normal diet, such as various forages and even grains. In some, they react to almost every forage type and grain. If this were true and indeed the problem, what are they supposed to eat? We can modify those diets, introduce foreign and man created proteins and food stuffs, but rarely does this resolve the allergy.
What this is a sign of, is more so a hyper-responsive immune system, simply so out of balance that it is reacting with almost everything. Like an irritated adult that has had a bad day at work, then taking it out and reacting to their spouse, children or even the parking clerk. It more so helps us to see the scope of the problem, which is not a bad thing, but does come with a price. What is interesting in many of these cases, is that most of these patients can continue to consume those ‘reactive’ forages with little negative impact, after the condition is properly managed at a root level. Many owners are afraid that their horse is allergic to alfalfa, as an example, and eliminate it from the diet. After the condition is managed at a root level, the horse can actually eat that alfalfa in most cases, with no ill impact. You have to also remember that by eliminating certain forages from the diet, you are also eliminating nutrition which is vitally needed by the body. So, in some cases, we may actually be doing more harm than good through depriving the body of sustaining nutrients. Then we think we can replace these nutrients through a synthetic based supplement. It’s not that simple.
Allergy hypersensitivity injections work along the same lines and produce poor results in most patients. It is a good theory, overall, but benefits are not commonly achieved, resulting in resolution to the horse. Most horses receive these injections life long and a high percentage of those horses still exhibit allergy symptoms, sometimes unchanged in severity while in others, worse. Here again, the theory is correct, targeting the immune response, but overall, it is not addressing the root problem. Thus, results are highly variable and do come with a price tag.
Other therapies that address clinical signs more than the root cause include use of antihistamines, corticosteroids, topical skin creams, eye medications and bronchodilators to open airways. The bottom line with these medications is that they only address clinical symptoms and do very little for the underlying problem in that patient. As a result, the allergy condition often continues to worsen from year to year, requiring more medications, higher doses, creating more damage to the body.
What about the horse’s overall health that has allergies?
This is a good question and should be of concern on some level. An allergy is a sign of an improperly functioning immune system and also the presence of unbalance inflammation. One can influence the other, creating the other. An immune response that is over-reactive, triggers damaging inflammation. However, if the patient has a higher level of inflammation present, due to stress, diet, injury or other factors, that too can trigger an inappropriate immune response. This is why it is not uncommon to have a patient that seems to be ‘falling apart’, coming down with multiple problems then on top of it, this year developing allergies. They are all connected.
In seeing this, hopefully, we can also see that the presence of allergies should be a sign of general health imbalance in that patient. Through this, we should see that health is not optimal and allergies could just actually be a symptom of yet a bigger problem. We may have a patient with lameness issues and also recent allergy development, but if we focus on each problem as a single entity, we lose the game. If we put them together, seeing the bigger problem, our success rate increases.
Managing Equine Allergies for Optimal Results
That is the key question on everyone’s mind…how to best manage allergies? How can I make them go away? Unfortunately, there is no specific answer because the underlying cause or contributors can be different from one patient to the next. Each requires an individualized approach for best outcome. In all cases, we have to keep in mind two factors: inflammation and immune response. If we target our approach to balancing both, the outcome will be better and in most, medications are no longer needed.
First step…modifying the diet. In most cases, we have two culprits when it comes to the diet. Either they are not getting optimal nutrition to fuel the body and cell function, or they are receiving their nutrition in the form of synthetic based supplements. Both are detrimental to health, in my opinion. There is only one thing that truly provides what we are seeking and that is REAL FOOD, which includes herbs. Providing suboptimal nutrition, through poor quality hays or forage, depletes the body of nutrients that support normal health and balance. Using synthetic based supplements loaded with sugars, sweeteners, additives, preservatives and dyes can create more harm. The GI tract recognizes synthetic based nutrients in some cases as a foreign invader, which contributes to inflammation and immune problems locally. The additives, preservatives and other fillers are likewise seen as invaders, something that is not normally encountered, again adding to the problem. Couple that with more advanced leaky gut syndrome and these foreign proteins and chemicals can now potentially enter the blood circulation, triggering a systemic inflammatory response in that patient. Contributing to more harm, than providing good. We need to move to high quality forage in these patients and towards whole, natural grains when needed. We also need to implement the right herbs, not only for nutritional purposes, but also for medicinal value. This is what we refer to as cleaning up the diet.
Second step. . . improve digestive health in your horse. This is partially addressed by the dietary changes, as when you make these changes away from a processed food diet, you are removing chemicals and other additives which may be irritating digestion. What you need to do now is modify inflammation in the digestive tract and impact the microbiome. One main formula we rely on in this instance is the Ayurvedic herbal blend called Triphala, which is contained in the Cur-OST EQ Tri-GUT. This is a nice herbal blend that targets the digestive system by impacting inflammation, benefitting the microbiome, and helping to repair the leaky gut situation. In addition, I will often use a nice prebiotic blend of soluble and insoluble fiber to promote health in the microbiome. The main formula that I will use is the Cur-OST EQ Pro-GUT. Together, these two blends can go a long way to modify digestive health, inflammation, impact allergies and improve the overall health of the horse. As far as I am concerned, as a veterinarian, every horse should be on at least one of these two products. That is how important digestion is for equine health.
Third step…modify the inflammatory and immune response. This is done partially by changing the diet. As you move towards more whole or real foods, away from chemicals and synthetics, the body is healthier, inflammatory levels reduced and immune response more balanced. You are reducing a contributor through dietary changes. This is also where herbs come into play, being used primarily for their medicinal properties to help balance the inflammatory response, immune response and promote cellular healing. Herbs can be very beneficial when used properly, healing underlying damage and promoting overall health. The herbs chosen cannot just impact inflammation as a whole concept, but used to target specific areas such as the gut, promoting health and balance in that region. There are many options in this step, but the two main blends we will utilize are either the Cur-OST EQ Immune Support or the Cur-OST EQ Total Support. I tend to lean towards the later of the two in more severe or chronic allergy situations in the horse.
Fourth step…modify stress. Stress, mental and physical, play a huge role in the immune response. An exaggerated stress response results in excess cortisol production and changes in other hormones along the HPA axis, which can then influence immune response and inflammation. There are many contributors to stress, not just the obvious such as prolonged stall confinement. An improper diet also can create stress internally, cellular stress. A concurrent lameness or health problem also creates stress, internally. We have to support that stress response, reduce it, control it better. This can be through reduction of the ‘stressor’, but also through dietary changes, training changes, and proper use of herbs. I generally try to modify lifestyle and other controllable factors first, then if needed, I will add in various herbs to impact this process. The main blend I will utilize is the Cur-OST EQ Adapt & Calm.
Through all of these steps, you have two primary goals; restore/balance health and also reduce contributors. If you can eliminate a contributor, an allergen, then you will be able to better manage the process. Likewise, if you support health on a cellular level, you also are able to better manage the process, as then the body is more balanced, capable of a proper response and also capable of repair.
Through the use of proper diet, herbal formula uses and stress reduction, a high percentage of patients respond readily. One thing to keep in mind is that there are many contributors to a problem, and sometimes we gain improvement but desire more. In those cases, we need to further evaluate, make sure there is not a contributor still in play. In other cases, we have to remember that the health imbalance has been present for quite some time, years actually, in many horses. There is a tremendous amount of damage that needs repair and rebalancing, which may take more time. I think that in most patients, one error that we do make is assume the problem is ‘cured’ when clinical signs improve or resolve. We also tend to lose focus on that allergy condition, thinking it is gone, as the season or weather changes. Both are incorrect. Improvement in clinical signs is great and a goal, but if we back off of support to that body, many times it returns, sometimes worse. Health is not just gained…but maintained. Weather and seasons are strong influencers of allergies, making them more readily apparent, making the pot boil over. Just because the season has changed and condition has improved, does not mean the underlying health imbalance is not present. It is still there…just not being pushed to the maximum. Daily regimens, used throughout the year, from diet to stress to herbs should be employed at all times for the best possible outcome.
Allergies can be managed, for the better, when the right approach is put into play. When we see the bigger problem, the approach may seem complex, but in reality, it is simple. In the end, we can not only improve the allergies, but overall health and even performance for that patient.
Author: Tom Schell, D.V.M., CVCH
Further Reading:
Managing Allergies in the Horse – SecondVet


Hi Dr Schell.
My 19 yr old Quarter horse started having teary eyes about 3 years ago. The wind seemed to be the primary reason in the summer. However, last winter his eyes continued to tear. A fly mask doesn’t seem to help in the summer. He is not Metabolic. I clean his eyes, sometimes twice daily with water and a paper towel. There are no signs of infection and I had his tear ducts flushed this spring with his vet check with no improvement. I have tried two 6 week courses of a Zinc supplement but have seen no improvement. Is there something else I can try and/or should he have an opthamalogic exam.
I have used several of your products for my Cushings/IR Arab mare which I am happy to report have resolved (via bloodwork results and clinical findings) along with diet changes and exercise over the past year.
I am hoping I can help my Quarter horse as well.
I look forward to hearing from you.
Sincerely,
Marsha